 Video Courses
Video Courses Video Courses
Video CoursesECG/EKG can be easily misinterpreted. We've put together a list of the ways to avoid this.
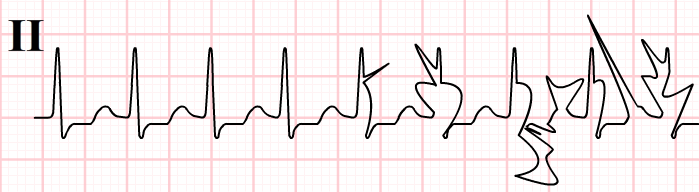
Modern ECG machines will present you with a computerized interpretation of the readout (‘the CI’). This computer diagnosis is frequently wrong (up to 20% of cases)! These errors can be critical, for example, many patients in sinus rhythm have been started on dangerous medications due to an erroneous computer diagnosis of atrial fibrillation. It has also been shown that the CI can give doctors a false sense of security and lead to interventions which would otherwise not have been carried out. We are not saying that the CI is of no use, in fact it can prevent error. However, it is a guide to your final diagnosis and nothing more than that.
ECGs should always be interpreted in clinical context. For example, the majority of people presenting to the ED with ST elevation on their ECG, even those with chest pain, are not having a myocardial infarction.
It follows from tip number 2 that you should make yourself very familiar with the nuances of the ST segment in health and disease.
Generation of a normal ECG depends on correct placement of the ECG electrodes on the patient's body. Electrode misplacement when recording an ECG is a common error. You will find yourself standing in front of a patient with a confusing looking ECG and wondering ‘could the electrodes have been misplaced’ and wishing you knew how to tell! Understanding, how to identify electrode misplacement requires a knowledge of a few simple principles outlined in the normal ECG course on acadoodle.com.
There are twelve ‘leads’ on an ECG readout for a reason. The ECG machine is capable of analysing the flow of depolarisation and repolarisation around the heart from 12 different perspectives. In a given individual an electrical event in the heart may be ‘seen’ (that is recorded) by one lead but not by another. This can have critical implications in a given case. For example, when diagnosing arrhythmias, detection of atrial depolarisation in a ‘less fashionable’ lead can change everything. We show you how this works when dealing with arrhythmia diagnosis in ECG section 4 on acadoodle.com.
Finally, remember the ECG is not easy. Even experts who spend their lives looking at ECGs get a significant proportion of ECG diagnoses wrong, particularly when analysis takes place outside of clinical context. When asked about a patient’s ECG on a post call ward round, one of my Senior House Officer’s once told me that she had given up on ECGs ‘because they never look the way they’re supposed to’. There is some truth in this statement and in practice it takes years of experience to develop confidence in ECG diagnosis. However, you have to start somewhere and the ECG section on acadoodle.com will give you a good foundation on which to build your knowledge of ECGs.
Check out our video course on Avoiding Error in ECG Diagnosis
DisclaimerPrivacy PolicyTerms of UseData Deletion© Acadoodle 2026